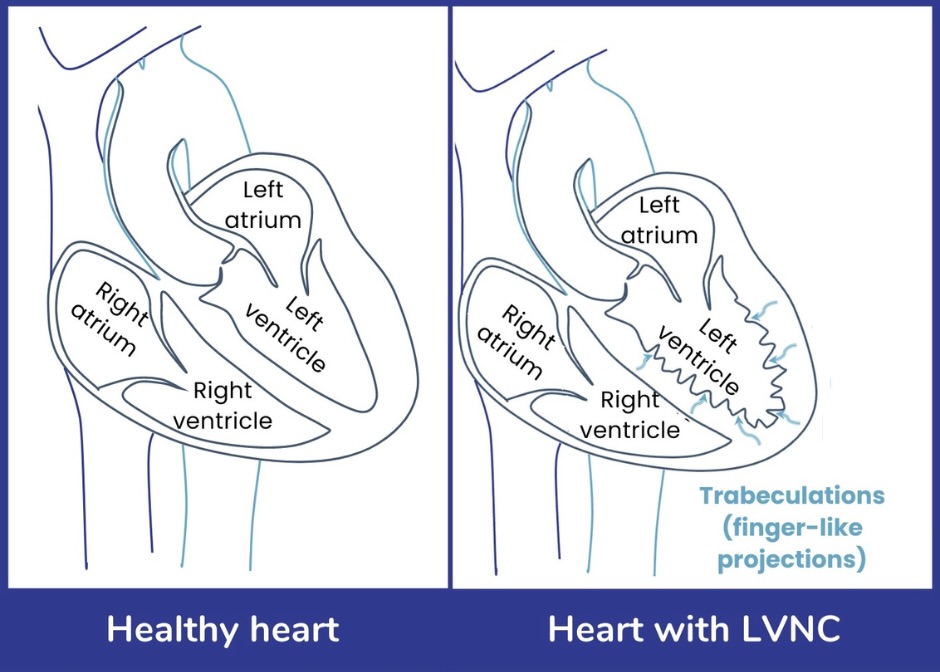
Left-ventricular non-compaction cardiomyopathy (LVNC) is a condition that affects the muscular wall of the left ventricle (bottom part) of the heart. LVNC can occur as an isolated heart condition, or with other heart problems. Sometimes trabeculations can be a normal finding in healthy people and not considered disease. LVNC usually occurs during the development of the heart before a person is born, but can develop after birth.
This page focuses on inherited LVNC, but people with other kinds of LVNC may find this useful.