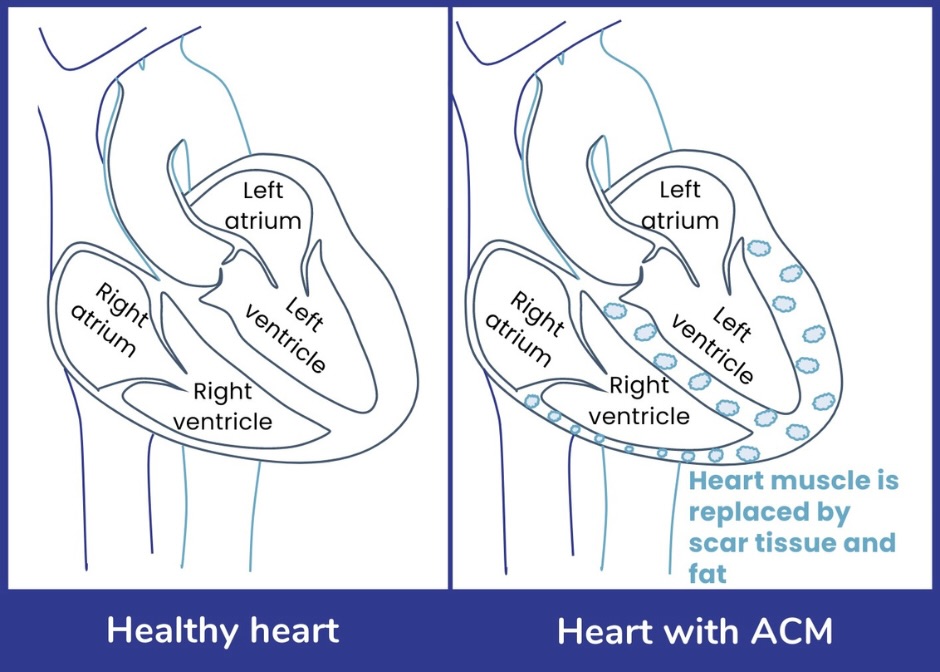
Arrhythmogenic cardiomyopathy (ACM) is a heart condition that affects the muscle in the heart. The heart is made up of four chambers. The bottom two chambers are called the ventricles. The ventricles are the pumping chambers of the heart which send blood out from the heart and around the body. ACM can affect the right or left ventricle of the heart, or both.
ACM is an inherited condition, meaning it is caused by a genetic change present at birth that can be passed down through a family.